Key Takeaways
- Medicaid coverage is expanding rapidly, increasing access to both exome and genome sequencing.
- State decisions drive real-world impact, with large markets like Texas and emerging adopters like Maine and Arkansas.
- States are adding exome and genome coverage at different speeds, creating variation in what patients can access depending on where they live.
Medicaid Genomic Coverage More Than Doubles—With Texas and Other States Leading the Way
Access to genomic testing can be life-changing—ending diagnostic odysseys, guiding clinical care, and connecting patients to targeted treatments. But even with the science in place, access ultimately comes down to insurance coverage.
While coverage of exome sequencing has been nearly universal across commercial insurance plans for several years, Medicaid lagged in most states. Recent momentum in Medicaid coverage marks an important step forward in closing disparities and making genomic testing more accessible to the patients who need it most.
Coverage as a Driver of Equity
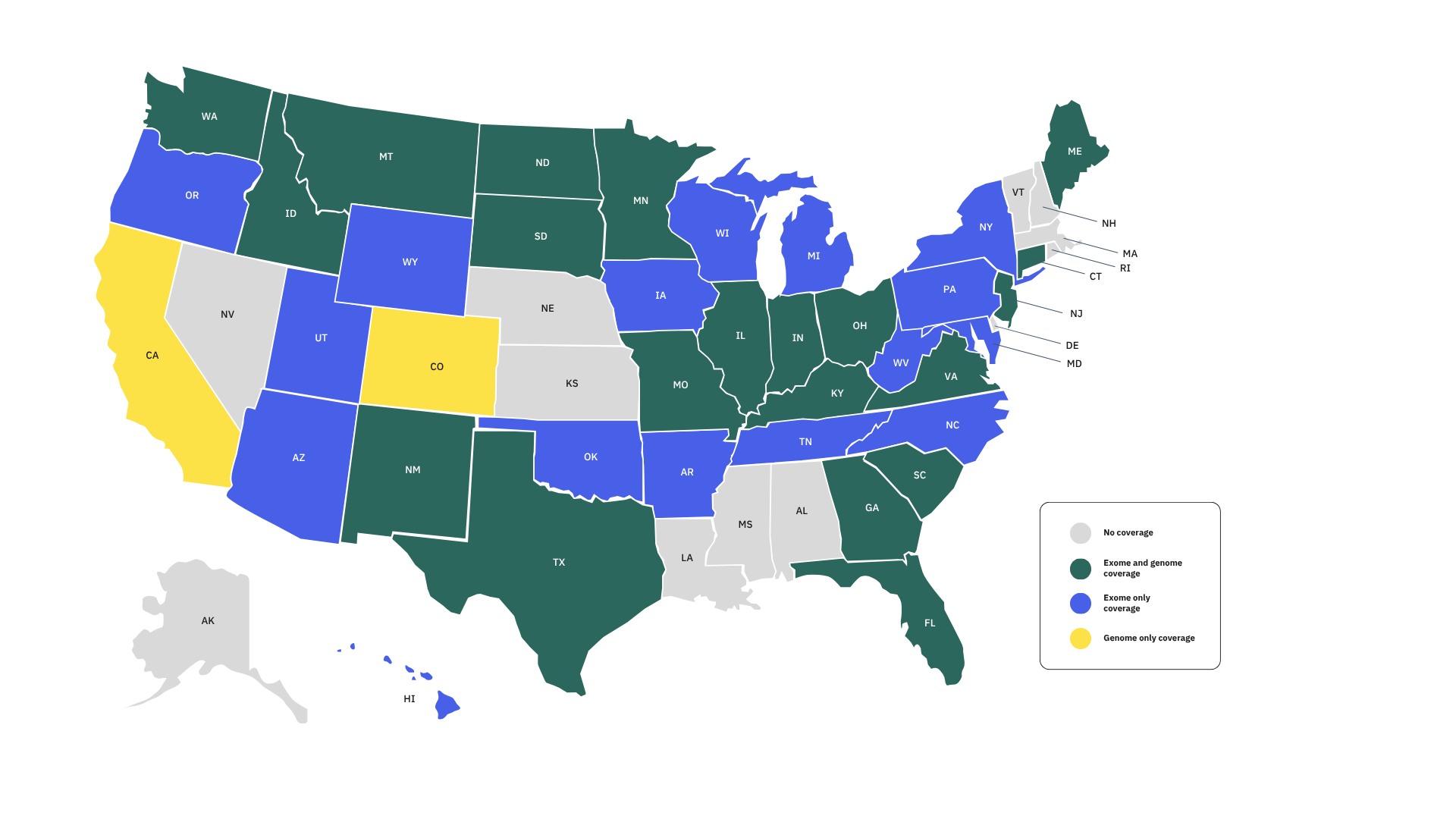
According to new research presented by GeneDx's Sarah Soto, MS, CGC, at the 2026 PLUGS Summit (From Evidence to Access: a Year of Progress in Exome and Genome Sequencing Payor Coverage), Medicaid coverage for genomic testing has expanded rapidly over the past year. Soto, Medical Policy Impact and Payor Evidence Strategy, at GeneDx, shared that genome sequencing coverage grew from 28% to 66%, while exome coverage increased from 49% to 70%. Today, 38 states offer Medicaid coverage for outpatient exome and/or genome sequencing.
Medicaid plays a critical role in covering children with complex medical needs, yet advanced genomic testing has historically been more difficult to access for those insured by Medicaid.
That gap is beginning to close.
This progress reflects a broader shift: clinical guidance, including from organizations such as the American College of Medical Genetics and Genomics (ACMG) and the American Academy of Pediatrics (AAP), already recommend exome or genome sequencing as first-line testing in many cases. Coverage is now catching up to the standard of care.
Texas: A Leading Example of Progress
Texas stands out as a leading example of how Medicaid programs are advancing access to genomic testing at scale.
In September 2024, Texas Medicaid became an early mover by covering whole genome sequencing (WGS) in the outpatient setting—demonstrating a strong commitment to bringing advanced diagnostics to its population. More recently, the state expanded its coverage to include exome sequencing (ES), effective May 1st.
Together, these decisions mark a significant step forward for one of the largest Medicaid populations in the country. By enabling access to both exome and genome sequencing, Texas is helping ensure that more patients can benefit from timely, comprehensive genetic insights that enable precision medicine.
A Broader National Trend in Medicaid Genetic Testing Coverage
Texas is not alone. Similar patterns are emerging across the country as states expand genomic testing coverage and refine their approaches over time.
Maine, for example, introduced coverage for genome sequencing in 2025, and recently paired it with exome coverage—reflecting a growing recognition that both modalities play a role in clinical care. While smaller in scale, Maine’s progression mirrors what’s happening nationally: states are not only adding coverage, but evolving policies to better align with how genomic testing is used in practice.
Moving Forward: Expanding Access Through Medicaid Coverage
The rapid expansion of Medicaid coverage is a clear signal of progress. But there is still work to be done closing the remaining gaps between access for those with commercial coverage and those insured by Medicaid.
Health plans have a unique opportunity to shape how genomic testing is delivered within their populations. Ending the diagnostic odyssey is not only good for patients and families, it is a public health imperative. GeneDx can provide thoughtful implementation support, market access expertise, evidence packets, and provider education. We are committed to ensuring that coverage translates into timely diagnoses, better care decisions, and improved outcomes for the patients who need it most.
%201.png)




